Международный эндокринологический журнал 1 (65) 2015
Вернуться к номеру
Peculiarities of Antithyroid Autoimmunity Indicators in Type 2 Diabetic Patients Depending on Leptin Level in Blood Serum and Their Dynamics as a Result of Sodium Selenite Treatment
Авторы: Abramova N.O., Pashkovska N.V., Berezova M.S. - Bukovinian State Medical University, Chernivtsi, Ukraine
Рубрики: Эндокринология
Разделы: Клинические исследования
Версия для печати
There were studied 46 patients with diabetes mellitus type 2 in order to identify the autoimmune processes directed against thyroid tissue and dependence of those changes on the level of leptin in blood serum. It was established that in patients with high leptin serum level antithyroid antibody titer increased. In order to adjust the levels of antithyroid antibodies sodium selenite was prescribed against the background of standard therapy. Statistically significant reduction in antibodies expression to thyroglobulin and thyroperoxidase after treatment with sodium selenite dosed 50 mg after a month has been found.
Обследовано 46 больных с сахарным диабетом 2-го типа на предмет наличия аутоиммунных процессов, направленных против ткани щитовидной железы, с целью выявления зависимости этих изменений от уровня лептина в сыворотке крови. Установлено, что у пациентов с высоким уровнем лептинемии возрастает титр антитиреоидных антител. С целью коррекции уровней антитиреоидных антител назначался препарат селенита натрия на фоне стандартной терапии. Установлено статистически значимое снижение экспрессии антител к тиреоглобулину и тиреопероксидазе в результате лечения селенитом натрия в дозе 50 мкг через 1 месяц.
Обстежено 46 хворих на цукровий діабет 2-го типу на предмет наявності автоімунних процесів, спрямованих проти тканини щитоподібної залози, із метою виявлення залежності цих змін від рівня лептину в сироватці крові. Встановлено, що у пацієнтів із високим рівнем лептинемії зростає титр антитиреоїдних антитіл. З метою корекції рівнів антитиреоїдних антитіл призначався препарат селеніту натрію на тлі стандартної терапії. Встановлено статистично значуще зниження експресії антитіл до тиреоглобуліну та тиреопероксидази в результаті лікування селенітом натрію в дозі 50 мкг через 1 місяць.
diabetes mellitus type 2, leptin, antithyroid antibodies, selenium.
сахарный диабет 2-го типа, лептин, антитиреоидные антитела, селен.
цукровий діабет 2-го типу, лептин, антитиреоїдні антитіла, селен.
Статья опубликована на с. 9-12
Introduction
During the last three decades the number of patients with type 2 diabetes mellitus (DM) have increased, which is associated with an increase in the prevalence of obesity among the world's population [6]. In recent years it has become known that adipose tissue is an endocrine active organ that produces cytokines, or adipokines. DM type 2 and obesity are closely linked with the production of adipokines by adipose tissue [8].
It was found that in obese patients level of leptin in the blood plasma increases significantly, it is associated with the accumulation of white adipose tissue on abdominal region an resistance of receptors to leptin action development. Also a direct correlation between the levels of serum leptin and insulin was found that indicate the impact of this adipokine on the insulin resistance (IR) development [10].
Leptin enhances production of proinflammatory cytokines such as interleukin–6, tumor necrosis factor, which adversely affect the energy metabolism and muscle tissue sensitivity to insulin, and liver [8].
Thyroid diseases as well as type 2 DM are the most common endocrine pathologies. Many studies have found an increase of antithyroid antibodies titers against the background of type 2 DM [11, 14].
Changes in the immune system may be exacerbated as a result of inadequate intake of selenium in endemic areas.
According to the literature data, a chronic autoimmune thyroiditis (AIT) affects 10 % of women and 20 % of male population. The pathogenesis of AIT is associated with decreased activity of selenium containing enzymes which protect the thyroid gland from oxidative stress and an increase in autoimmune processes, which are associated with selenium deficiency in endemic areas [9].
There is a low content of selenium in the soil on the territory of Ukraine, including the territory of Bukovina, where the selenium content in soil is 0.20 mg/kg — 0.60 mg/kg depending on the region [3]. Normal consumption of selenium is considered to be 50 mcg for women and 70 mcg for men per day, the maximum safety dose should not exceed 400 mcg, the recommended dose of selenium in the USA and Canada is 55 mcg/day [1].
In addition, according to some authors observations, on the background of type 2 DM and metabolic syndrome selenium consumption decreases [16].
But relationship between thyroid autoimmunity and concomitant type 2 DM is still understudied. And effective methods of immune system disorders in such patients yet have not been developed.
The aim of the study is to determine the characteristics of antithyroid autoimmunity in patients with type 2 diabetes mellitus, depending on the leptin level in blood serum and develop a method of the identified changes correction.
Materials and methods
46 patients with type 2 DM who were hospitalized in the Chernivtsy Regional Endocrinology center and Chernivtsi Regional hospital invalids of the Great Patriotic War were investigated.
To assess glucose metabolism we used the order of Ukrainian Health Ministry from 21.12.2012 № 1118 «About the approval and implementation of medical and technological documents on standardization of medical care in type 2 diabetes mellitus» [4].
To establish IR the level of immunoreactive insulin (IRI) was determined and HOMA–IR was calculated. In case of increase of IRI more than 25 IU/ml and HOMA–IR more than 2 IR was determined.
Serum leptin concentration of venous blood was determined to establish the pro–inflammatory activity of the adipocytes.
Depending on the leptin level in blood serum patients were divided into groups as follows: group I — level of leptin — less than 10 ng/ml (12 patients), group II — level of leptin within 10–25 ng/ml (19 patients), group III — level of leptin more than 25 ng/ml (15 patients).
Thyroid autoimmunity was diagnosed by antibodies to thyroid peroxidase (AT–TPO) and thyroglobulin (AT–TG) determination in the blood serum.
In order to evaluate the effectiveness of treatment, patients were randomly divided into two groups: 20 people with type 2 DM received standard treatment, which included oral hypoglycemic agents that refer to biguanide class (metformin in mean daily dose of 1000–2000 mg/day). The main group included 30 people who received «Tsefasel» which contains 0.333 mg of sodium selenite, which is equivalent to 100 micrograms of selenium, by tablet per day for 30 days against the background of basic therapy.
Statistical analysis of the obtained data was carried out using the Student’s t–test and Pearson's rank correlation coefficient by means of the software package Statistica 6.0 for Windows. The difference was considered reliable at p < 0.05.
Results and discussion
In order to identify autoimmune disorders we studied the level of AT–TG and AT–TPO. According to obtained data AT–TG level in group III was 2.1 times higher than in group I (p <0.05) (Table 1).
AT–TPO titers in groups II and III was 44.3 and 92.2 %, respectively higher than in group I (p < 0.05).
Enhancement of antibodies to thyroid tissue production may be due to the fact that elevation of leptin level is accompanied by a predominance of cell–mediated immune responses, due to increased production of cytokines by T–helpers type 1 against the background of decreased functional ability of T–suppressors and an increased number of natural killers (NK–cells) in obese patients with type 2 DM [5, 12]. Such changes in the immune system lead to thyrocytes alterations and apoptosis development and are characteristics of autoimmune thyroiditis [13, 17].
As a result of the correlation analysis, we found a positive correlation between leptin levels and antithyroid antibodies titers, namely AT–TG (r = 0.544, p < 0.05) and AT–TPO (r = 0.423, p < 0.05), immunoreactive insulin level in the blood serum and the content of AT–TG (r = 0.362, p < 0.05) and AT–TPO (r = 0.327, p < 0.05), HOMA–IR and AT–TG (r = 0.459, p < 0.05) and AT–TPO (r = 0.432, p < 0.05)
In addition to elevated level of leptin, abnormalities in the immune defense system may be due to the development of IR. It is known that insulin except basic biological effects, also has anti–inflammatory properties. Normally it inhibits several inflammatory transcription factors: NF–kB, AP–1 and genes that regulate them [8]. In case of resistance of receptors to insulin, this effect is not implemented and as a result transcription factors and pro–inflammatory cytokines may be activated, that cause thyrocytes damage.
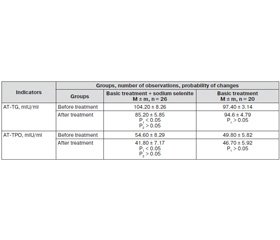
A significant improvement of indicators that reflect the autoimmune processes against thyroid tissue have been found only in the group of persons who took sodium selenite with standard therapy: the level of AT–TG became 22.3 % lower (p < 0.05) and AT–TPO — 30.6 % than before sodium selenite treatment (p < 0.05) (Table 2).
Autoimmune processes develop as a result of thyroid tissue damage, because of autoimmune protection violation due to the depression of T–suppressors production against the background of increased activity of T–helpers. Selenium supplementation contributes to the lipid peroxidation suppression by increasement activity of antioxidant enzymes and restores the balance of the immune system due to the inhibitory effect on HLA–DR system of thyrocytes. It is well known that some of the HLA system antigens stimulate the release of T–helpers with subsequent stimulation of antibodies expression by B–lymphocytes [1, 15].
Conclusions
1. In patients with type 2 diabetes mellitus an antithyroid antibodies titers increase.
2. Growth of antithyroid antibody titers in patients with type 2 diabetes mellitus is associated with elevation of leptin level and insulin resistance manifestations.
3. Significant decrease in antibodies to thyroglobulin and thyroid peroxidase titers in patients with type 2 diabetes mellitus against the background of sodium selenite intake have been observed.
1. Гончарова О.А. Ассоциативные связи между микоплазмой и компонентами иммунного ответа у женщин с аутоиммунным тиреоидитом [Текст] / О.А. Гончарова // Международный эндокринологический журнал. — 2014. — № 7(63). — С. 18–22.
2. Кравчун Н.О. Особливості антигіпертензивної терапії у хворих на цукровий діабет 2–го типу з метаболічним синдромом та її вплив на розвиток серцево–судинних ускладнень / Н.О. Кравчун, Т.С. Гринченко, Л.П. Доценко // Международный эндокринологический журнал. — 2008. — № 4(16). — С. 20–26.
3. Кравченко В.І. Дослідження впливу дефіциту селену на розвиток дифузного зоба в дітей Чернігівської області [Текст] / В.І. Кравченко, О.І. Осадців, І.М. Андрусишина // Ендокринологія. — 2012. — Т. 17, № 3. — С. 7–12.
4. Про затвердження та впровадження медико–технологічних документів зі стандартизації медичної допомоги при цукровому діабеті 2 типу. — Наказ МОЗ України № 1118 від 21.12.2012.
5. Салихова А.Ф. О роли цитокинов в патогенезе ожирения / А.Ф. Салихова, Л.М. Фархутдинова // Цитокины и воспаление. — 2013. — Т. 12, № 3. — С. 21–23.
6. Chen L. The worldwide epidemiology of type 2 diabetes mellitus — present and future perspectives / L. Chen, D.J. Magliano, P.Z. Zimmet [et al.] // Nature Reviews Endocrinology. — 2012. — Vol. 8. — Р. 228–236.
7. Coimbra S. Adiponectin, Leptin, and Chemerin in Elderly Patients with Type 2 Diabetes Mellitus: A Close Linkage with Obesity and Length of the Disease / S. Coimbra, J.B. Proença, A. Santos–Silva // BioMed Research International. — 2014. — Vol. 14. — Режим доступу до журн.: http://dx.doi.org/10.1155/2014/701915
8. Das P. Association of obesity and leptin with insulin resistancein type 2 diabetes mellitus in indian population / P. Das, D. Bhattacharjee, S. Kumar // Indian J. Physiol. Pharmacol. — 2013. — Vol. 57(1). — P. 45–50.
9. Duntas L.H. Selenium and the thyroid: a close–knit connection / L.H. Duntas // J. Clin. Endocrinol. Metab. — 2010. — Vol. 95, № 12. — P. 5180–5188.
10. Ginter E. Diabetes type 2 pandemic in 21st century / E. Ginter, V. Simko // Bratislavské lekárske listy. — 2010. — Vol. 111, № 3. — Р. 134–137.
11. Hajieh S. Prevalence of thyroid dysfunction and thyroid auto antibodies in type 2 diabetic patients / S. Hajieh, M. Behbahani, A. Mohtashami // Pak. J. Med. Sci. — 2011. — Vol. 27, № 5. — Р. 1169–1172.
12. Kostitska I.O. Аutoimmune thyroiditis associated with metabolic syndrome in postmenopausal women / I.O. Kostitska, I.G. Babenko // Maturitas. — 2012. — Vol. 71, Supplement 1. — Pages S78–S79.
13. Marzullo P. Investigations of Thyroid Hormones and Antibodies in Obesity: Leptin Levels Are Associated with Thyroid Autoimmunity Independent of Bioanthropometric, Hormonal, and Weight–Related Determinants / P. Marzullo, A. Minocci, M.A. Tagliaferri // Clin. Endocrinol. Metabol. — 2010. — Vol. 95, № 8. — P. 3965–3972.
14. Palma C. Prevalence of thyroid dysfunction in patients with diabetes mellitus / C. Palma1, M. Pavesi, V. Guedes Nogueira // Diabetology and Metabolic Syndrome. — 2013. — Vol. 5, № 58. — Режим доступу до журн.: http://www.dmsjournal.com/content/5/1/58
15. Smith A.D. Selenium status alters the immune response and expulsion of adult Heligmosomoides bakeri in mice / A.D. Smith, L. Cheung, E. Beshah et al. // Infection and immunity. — 2014. — Vol. 82, № 1. — Режим доступу до журн.: http://iai.asm.org/content/early/2013/04/30/IAI.01047–12.
16. Kornhauser C. Serum selenium and glutathione peroxidase concentrations in type 2 diabetes mellitus patients / C. Kornhauser, J.R. Garcia–Ramirez, K. Wrobel et al. // Prim. Care. Diabetes. — 2008. — Vol. 2, № 2. — P. 81–85.
17. Tamer G. Effects of thyroid autoimmunity on abdominal obesity and hyperlipidaemia / G. Tamer, M. Mert, I. Tamer // Endokrynologia Polska (Polish Journal of Endocrinology). — 2011. — Vol. 62, № 5. — P. 421–428.

/10/10.jpg)
/11/11.jpg)